The diagnostic value of body temperature has been known for centuries. Disorders such as encephalitis (symptoms: fever, tremor, seizures, confusion, delirium, anxiety and vomiting) were even described by Hippocrates and Galenos in ancient Greece. Body temperatures that are too high or too low affect metabolism, metabolic processes and organ function and can even damage tissue.
Infrared thermography has long been used in veterinary medicine as a routine diagnostic procedure (see the book by Barbara Bockstrahler MD: Physical medicine, rehabilitation and sports medicine in a nutshell – VBS (publisher) 2019). In just a few seconds it allows the visual assessment of internal inflammation in animals, compensating postures, impaired gait, hoof disorders, painful pressure points and muscle and joint inflammation. Based on these findings in veterinary medicine, we began to use this procedure two years ago in the diagnostic assessment and rehabilitation of muscle injuries in professional football and have now also integrated infrared thermography as a complementary imaging procedure into our routine clinical practice for the clarification of musculoskeletal and neurological disorders. Case studies follow below as an illustration.
Case Studies
Case 1 (see Figs. 1 + 2)
presented with pain around the insertion of the right Achilles tendon. Clinical examination and imaging (ultrasound, X-ray and MRI) showed Haglund’s deformity with a partial tear in the deep layers of the Achilles tendon at the calcaneal insertion. Under ongoing treatment, the patient complained of sciatica on the right without a sensory motor deficit after returning to full sports loading. Clinical examination and imaging showed a facet joint cyst at L4/5 on the right with marked narrowing of the spinal canal on the right and nerve root compression at L5 and S1 on the right.
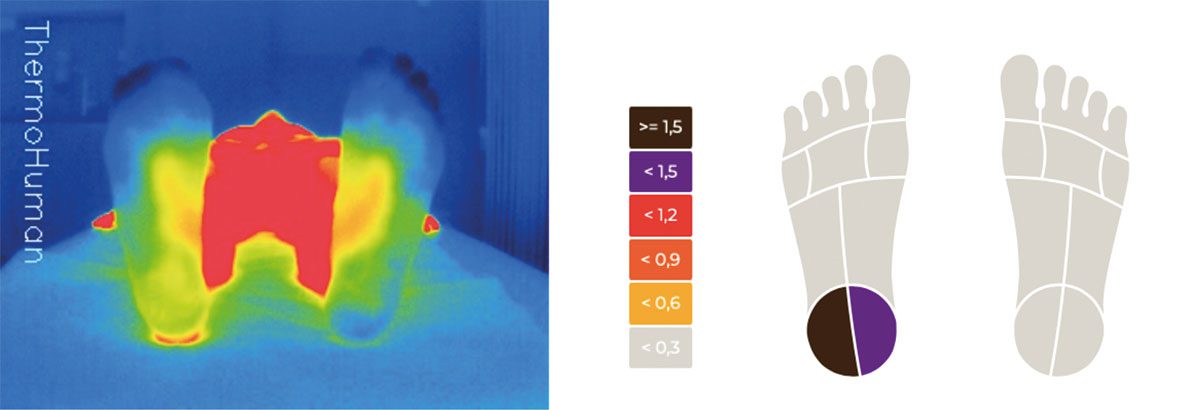
FIG. 1 Infrared thermography of the soles of both feet. Thermographic images assessed using the Thermohuman software, camera: X4VIson by HT ITALIA SRL. Temperature difference between the right and left heel, 2.19°

resection of a facet joint cyst at L4/5 on the right. Although the patient was entirely free of pain,
a temperature difference between the medial left and right gastrocnemius was still detectable (1.2 – 1.5°).
Temperature around the Achilles tendon insertion and the heel markedly warmer on the right than on the left (2.5°)
Case 2 (see Fig.3)
A 34-year-old male patient with bilateral cam-type femorocetabular impingement. Due to the lack of success under conservative treatment, hip arthroscopy was performed on the right with debridement of the torn labrum and offset restoration (removal of a bony hump).

Case 3 (see Fig. 4)
An 80-year-old female patient with activated osteoarthritis on the left confirmed by imaging and immobilising pain under weight-bearing. Alleviation of the symptoms under conservative treatment.

Case 4 (see Fig. 5)
A 48-year-old male runner with ongoing heel pain for the previous six months. Clinical examination and imaging (MRI) confirmed the diagnosis of plantar fasciitis with a degenerative partial tear of the plantar tendon at the calcaneal insertion.

Conclusion
Infrared thermography provides us in our orthopaedic and sports medicine practice with a complementary imaging procedure that is fast, non-invasive, painless, objective and above all radiation-free. The colour-coded visualisation of slight differences in skin temperature and the specialist Thermohuman software (camera: X4VIson by HT ITALIA SRL) allow assessment of thermographic images that is easily standardised. In an online article in the sportärztezeitung, the sports scientist Kornelius Kraus MD wrote about his many years of experience in infrared thermography as an assessment method for sports medicine and performance physiology (www.sportaerztezeitung.com/rubriken/therapie/10735/infrarotthermografie/). This included the finding that pain correlates with coordination deficits and that the ability to relax was poorer in the warmer hamstrings (Kraus 2019). To date, the diagnostic interpretation of the images depends to a great extent on the investigator and requires experience. In our view, infrared thermography has the potential of becoming a valuable and innovative complementary imaging procedure in orthopaedics and sports medicine alongside established diagnostic procedures such as ultrasound, MRI and electromyography. To date, there have been no randomised prospective studies comparing the informative value of this procedure with that of other imaging procedures. Well-designed studies are required to further investigate the value of this imaging procedure in musculoskeletal diagnostics.
Autoren
ist Facharzt für Orthopädie und Unfallchirurgie mit den Zusatzbezeichnungen Sportmedizin, Manuelle Therapie, Spezielle Unfallchirurgie und Spezielle Orthopädische Chirurgie. Er besitzt als Wirbelsäulenchirurg seit 2017 das Masterzertifikat der Deutschen Wirbelsäulengesellschaft (DWG) und ist seit 2021 gemeinsam mit Dr. med. Philipp Appelmann leitender Arzt des GALENOS in Mainz. Außerdem ist er seit 2012 Mannschaftsarzt des 1. FSV Mainz 05 und wiss. Beirat der sportärztezeitung.




