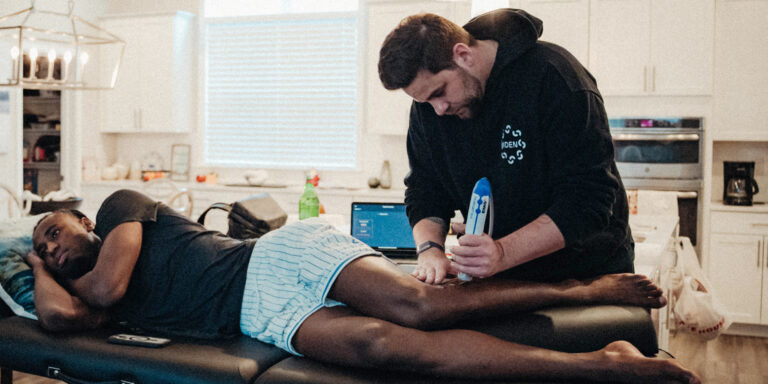
With an incidence rate of around 20%, supination trauma is the most common injury in basketball. Pre- and rehabilitation are therefore highly significant, and structured planning and precision are recommended. The case study presented here clearly shows how the combined use of EMG and radial shock waves can accelerate the rehabilitation process and lead to lasting success.
Aaron Nesmith, a player for the Indiana Pacers in the NBA, presented for the first time during the 2023/24 season playoffs with repetitive ankle problems, with a condition following multiple inversion traumas in the respective season. The initial diagnosis via EMG (myoact) showed clear deficits in the control of the peroneal muscles. The subsequent combination of osteopathy, manual therapy, and targeted facilitation via EMG biofeedback, partly with the aid of a blackboard, led to immediate improvement and ultimately to a convincing performance by the athlete until the Eastern Conference Finals of the season. Unfortunately, I was unable to continue treating the athlete during the off-season due to my work as a physical therapist for the national basketball team at the Olympic Games in Paris.
A new assessment was therefore carried out at the beginning of the current 2024/25 season, with unsatisfactory results. The control of the peroneal muscles, i.e., M. peroneus longus, had fallen to a balance score of 38 % in a right / left comparison, with an MVA on the affected left side of 141 mV compared to a near-optimal value of 367 mV on the right side. The data was consequently forwarded to the Indiana Pacers medical team with a request to jointly develop an appropriate treatment strategy to prevent further recurrences. Unfortunately, a significant recurrence occurred on the following game day with a combination trauma and partial ruptures of the retinaculum peroneale and both peroneal tendons.
This event required a rethinking of the treatment approach in order to ensure not only a timely but also a long-term successful return to play. The team initially considered surgical intervention to restore continuity, particularly of the peroneal retinaculum, but after consultation with colleagues, this was rejected in favor of a conservative treatment approach.

Conservative treatment approach & return to play
In order to determine the rehabilitation process for the subsequent subacute phase after conservative treatment in the acute phase, it was imperative to perform another EMG mapping via Myoact to establish the baseline. A further expected decline in control was observed, with 87 mV on the left vs. 344 mV on the right. In order to accelerate the control and reintegration of the affected muscles and to treat damaged tendon and ligament structures in a targeted manner, extracorporeal shock wave therapy (ESWT) from EMS was used. The high energy density enabled by the device is unique and was the decisive factor in this case. The athlete was advised against taking Celebrex (the standard medication in the NBA after trauma) due to reduced gene expression of scleraxis, collagen I, and III, and instead received supportive anti-inflammatory treatment with phytopharmaceuticals (curcumin and boswellia). This also ensured that the ESWT treatment in the ligament and tendon area was successful. The rest of the rehabilitation process consisted of both manual therapy and osteopathic elements to restore functional synergy, as well as training therapy measures with the aid of biofeedback training via EMG. ESWT was always used before training therapy with 3,000 – 4,000 pulses, divided between the muscular part of the peroneus longus, the retinaculum peroneale, and the peroneal tendons, at intervals of four to five days. The intensity was continuously adjusted to ensure the continuous release of substance P for the treatment to be successful. A significantly increased response and associated increased effectiveness of the subsequent training load was observed. This was graphically illustrated at regular intervals with EMG mappings comparing pre- and post-treatment, thereby confirming the long-term success of the ESWT application.
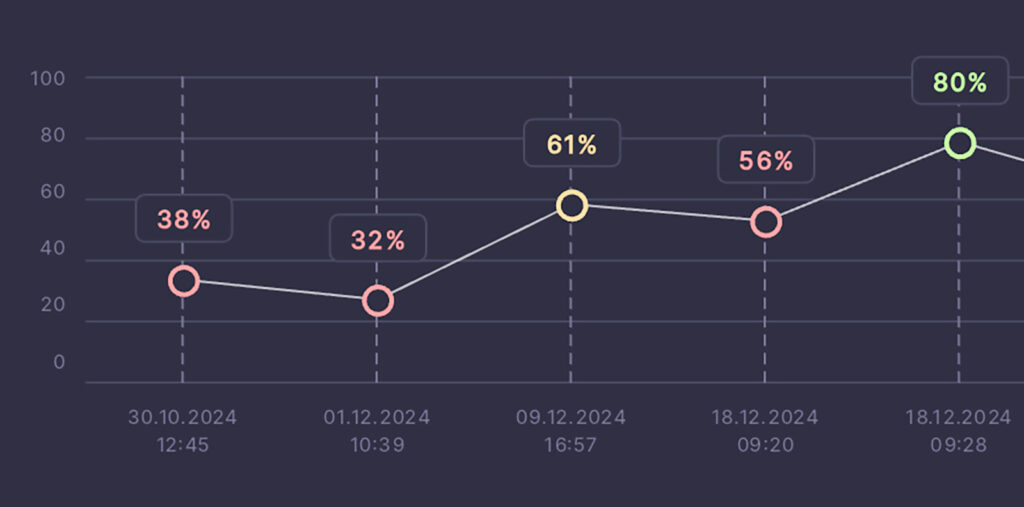
Return to play can only be successful if the athlete can restore confidence in the injured structure. The highly competitive nature of competitive athletes in particular benefits from graphical representations of their training and success progress, ensuring compliance throughout a demanding rehabilitation program, but also helping us therapists to be honest. The most striking comparative measurement was taken after the first ESWT application, around two and a half weeks after the trauma. The success of the treatment could be clearly deduced from an increase in the balance score from 56 % to 80 % and from 133 mV to 280 mV (left) via EMG. In the following sessions, the average balance score did not fall below approximately 70 % and a continuously adequate control could be established. In general, a balance score of over 80 % is not necessarily expected or required for a basketball player due to the differentiated load requirements in the left/right comparison, as long as sufficient control in the 400 mV range is guaranteed. This was achieved after about four weeks of rehabilitation, and the player was able to participate in contact-free on-court activities again. In the following weeks, targeted load control led to the desired results, but was deliberately designed to be slow and gradual. His return to play comeback was not marked by any setbacks, enabling the athlete to play one of his best seasons to date and currently rank among the top 10 three-point shooters in the NBA. This is particularly noteworthy because successful three-point shooters depend on perfectly coordinated mechanics in their ankle joints.
Autoren
ist Osteopath und Sportphysiotherapeut, der mit NBA-Athleten in den USA arbeitet. Dabei hat er spezielle Behandlungsprogramme für NBA und WNBA-Athleten entwickelt und umgesetzt, darunter All-Stars wie Pascal Siakam, Lauri Markkanen und Satou Sabally und konnte Verletzungen durch die Korrektur biomechanischer Bewegungsmuster wirksam vorbeugen. Außerdem ist er Teil des medizinischen Teams der deutschen Basketball-Nationalmannschaft, u.a. beim WM-Sieg 2023.