Prof. Dr. Robert Schleip / Technical University of Munich, Germany, TUM School of Medicine and Health, Emanuel Strüber, MD, Athanasia Georgiou, Myles Pistor / Clinic for Multimodal Pain Therapy, KRH Klinikum Region Hannover, Salah Layka, MD / Neurosurgery, Harzklinikum Dorothea Christiane Erxleben GmbH
Chronic pain after surgical procedures affects up to 30 – 50 % of patients who have undergone surgery and represents a significant challenge, including in follow-up care [1]. Scar tissue after lumbar spine surgery in particular can contribute to persistent pain due to increased tissue stiffness, reduced mobility, and nerve irritation [2]. The visible skin scar is only the “tip of the iceberg,” as fibrotic changes can continue deep into the tissue layers and affect nerve structures [3]. The aim of this study was to investigate the influence of microneedling on objective tissue parameters and subjective pain reports.
Study design and patient population
A prospective, descriptive observation was conducted. Thirty-one patients aged > 18 and < 80 years were included. All patients had chronic painful scarring for at least six months following surgery on the lumbar spine. Patients < 18 and > 80 years of age, with psychosomatic illnesses and secondary diseases that would have made it difficult to causally attribute the pain symptoms, were excluded.
- Gender: 71 % female
- Median age: 57 years
- Average BMI: 28.7 kg/m²
- Observation period: 12 days (T1–T2)
Intervention
Treatment was performed using microneedling (Dermaroller®, Medical Device MC910 1.0 mm) in the area of the postoperative scar tissue with a force of approximately 2 newtons and a rolling speed of 10 cm per second.
Ten repetitions were performed in each direction on the scar tissue, as well as 0.5 mm to the right and left of the scar tissue along the scar. This application was repeated a total of three times per patient during the twelve days of inpatient stay.
Measurement methods & statistics
Tissue stiffness: Of the five device-specific measurement parameters of the Myoton Pro, we selected the parameters Dynamic / Stiffness and Tone / Frequency in this study, as both parameters are best suited for indirectly determining tissue stiffness. The measurements were taken on the left, center, and right sides of the scar at fixed tissue markers. Indirect tissue stiffness was measured before the first treatment and one day after the last treatment. Pain intensity: A numerical rating scale (NRS 0 – 10) was used before the first and after the last intervention. The evaluation was descriptive.
Changes between T1 and T2 were represented by median values, and the NRS change was statistically tested.
Results
Dynamic/Stiffness (Fig. 2)
The measurements showed the following median changes between T1 and T2:
- Left: – 8.3 N/m
- Center: – 9.7 N/m
- Right: + 3.0 N/m
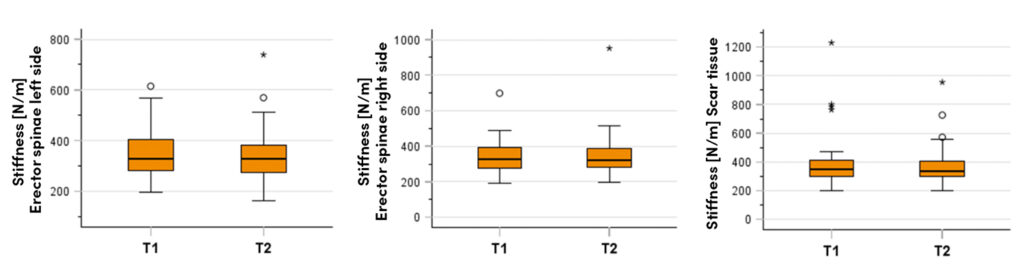
Tone / Frequency (Fig. 3)
Area LWS/erector spinae – left/right and scar area in T1 and T2 (descriptive)

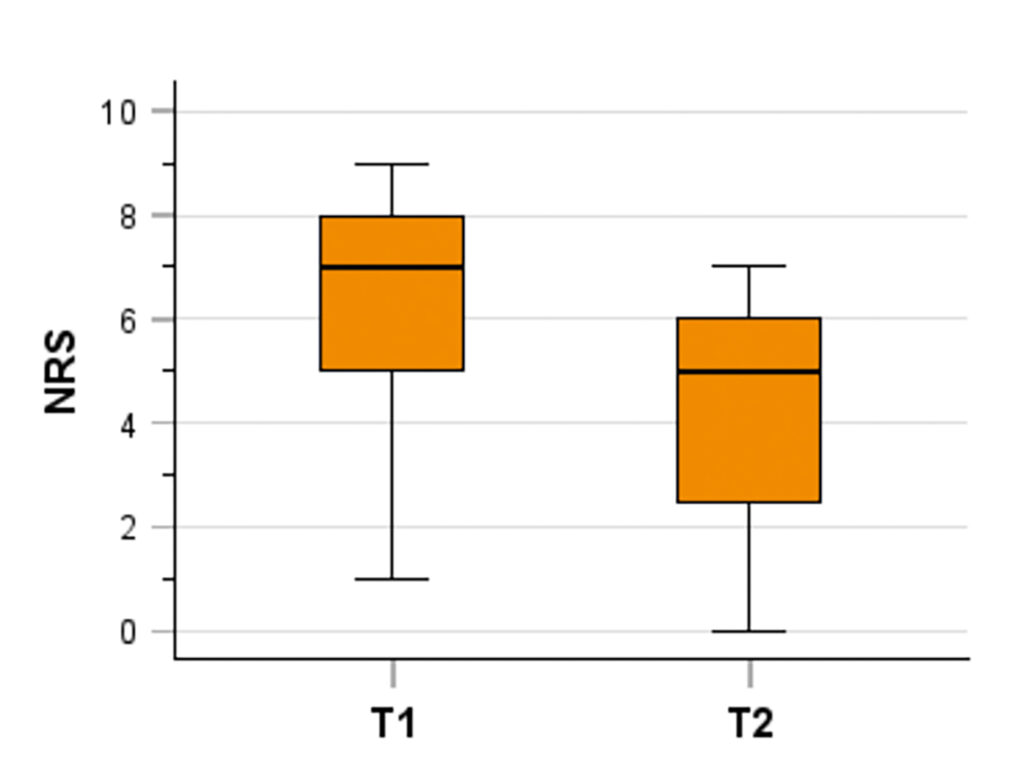
Pain intensity (Fig. 4)
The median NRS was 5 points in T2, which was significantly lower than in T1 with 7 points (Wilcoxon test for paired differences, p < 0.001). The NRS thus showed a significant reduction in pain intensity between T1 and T2.
Discussion & limitations
The results of this study suggest that microneedling can reduce scar-associated tissue stiffness. The observed reduction in pain is consistent with previous studies, which showed an improvement in scar-related parameters in up to 74 % of patients after microneedling [4, 5].
Whether altered tissue stiffness and improved pain symptoms can also positively influence tissue mobility and thus movement economy should be the subject of further studies. The limited number of cases and the absence of a control group limit the significance of the findings. In addition, this is a very limited observation in the context of standard inpatient therapies.
Conclusion for practice
Microneedling is a minimally invasive, easily integrated treatment option for chronic scar pain after lumbar spine surgery. The method leads to objective improvements in tissue stiffness and a significant reduction in pain intensity. Objective changes in tissue stiffness and a significant reduction in pain support its use in a comprehensive approach to scar-related pain. Microneedling can be an effective addition to a multimodal therapeutic approach for painful scar tissue. Randomized, controlled studies with functional endpoints are needed to confirm its full clinical relevance.
Literature
- Brown BC et al. The hidden cost of skin scars: quality of life after skin scarring. J Plast Reconstr Aesthet Surg. 2008;61:1049–1058.
- Tos P et al. Painful scar neuropathy: principles of diagnosis and treatment. Plast Aesthet Res. 2015;2:156–164.
- Choinière M et al. Pain and paresthesia related to scar tissue. Pain. 1991.
- Svenning M, Drejøe JB. Microneedling in mature burn scars. JMCRR. 2019;2:277–281.
- Abd-Elsayed A et al. Diagnosis, treatment, and management of painful scar. J Pain Res. 2022;15:1–12.
Conflict of interest: There is no conflict of interest.
Autoren
» MAMT. MT.POST GRAD (CH)., PT. BWL (HA)
» Institutsleiter am Institut für therapeutische Bereiche, Harzklinikum Dorothea Christiane Erxleben GmbH, Akademisches Lehrkrankenhaus der Otto von Guericke-Universität Magdeburg
» Gesamtverantwortliche Leitung Ambulante Medizin im Klinikverbund, Harzklinikum Dorothea Christiane Erxleben GmbH
(Stand 2026)