Gonarthrosis is one of the most common degenerative joint diseases. Intra-articular injections of corticosteroids offer effective and short-term symptom relief due to their potent anti-inflammatory effect. However, studies suggest that repeated steroid injections may be associated with an increased risk of cartilage damage and ultimately accelerated progression of osteoarthritis.
Parallel to steroid injections, hyaluronic acid injections have become established as a form of cartilage protection therapy due to their viscous supplementation effect. In recent years, the combined use of steroids and hyaluronic acid has become increasingly popular. The aim is to combine the rapid effect of steroids with the structural protective effect of hyaluronic acid.
The dilemma in practice: quick relief – long-term damage?
The strong anti-inflammatory effect of cortisone is undisputed and often leads to rapid clinical improvement in osteoarthritis, but this short-term solution has a downside. Research has shown that corticosteroids trigger the programmed cell death of cartilage cells [1] and that repeated injections therefore carry the risk of cartilage damage and accelerated osteoarthritis progression [2]. This circumstance presents practitioners and patients with the challenge that symptomatic relief could mask progressive structural damage to the joint.
Hyaluronic acid: More than just a lubricant
This is where hyaluronic acid (HA) comes into play, whose effect goes far beyond that of a pure “lubricant” for viscosupplementation. HA is a biologically active molecule with multiple functions in the joint:
- Mechanical protection: HA improves the viscoelastic properties of the synovial fluid, thereby providing mechanical protection for the joint surfaces.
-
Anti-inflammatory: HA modulates the inflammatory response, among other things by interacting with CD44 receptors on the cartilage cells, which inhibits the release of inflammatory mediators.
- Chondroprotection: HA directly protects the cartilage cells from the cell-damaging effects of steroids.
Preclinical and clinical evidence: What does the science say?
Combination therapy is a promising approach, whose synergistic effects have already been proven in several studies. A randomized, double-blind, placebo-controlled multicenter study from 2018 involving 368 patients showed that the combined administration of cortisone and hyaluronic acid led to significantly faster and more pronounced pain relief than the respective single therapies [3]. While the cortisone effect dominated in the first few weeks, the hyaluronic acid component provided lasting improvement for up to 26 weeks. The well-tolerated combination thus appears not only to enable effective short-term symptom control, but also to cushion the potentially adverse effects of cortisone on cartilage through the protective effect of hyaluronic acid, offering longer-term benefits. These clinical results are supported by several preclinical studies. In an in vitro model, bovine osteochondral tissue cultures were treated with inflammatory mediators (interleukin-1β and interleukin-17) to simulate an osteoarthritis-like environment [4].
The combined use of hyaluronic acid and glucocorticoids showed a significantly stronger inhibition of cartilage-degrading enzymes such as matrix metalloproteinases and proinflammatory cytokines compared to single doses. At the same time, the vitality of the cartilage cells was better preserved and there was a reduction in structural cartilage degradation.
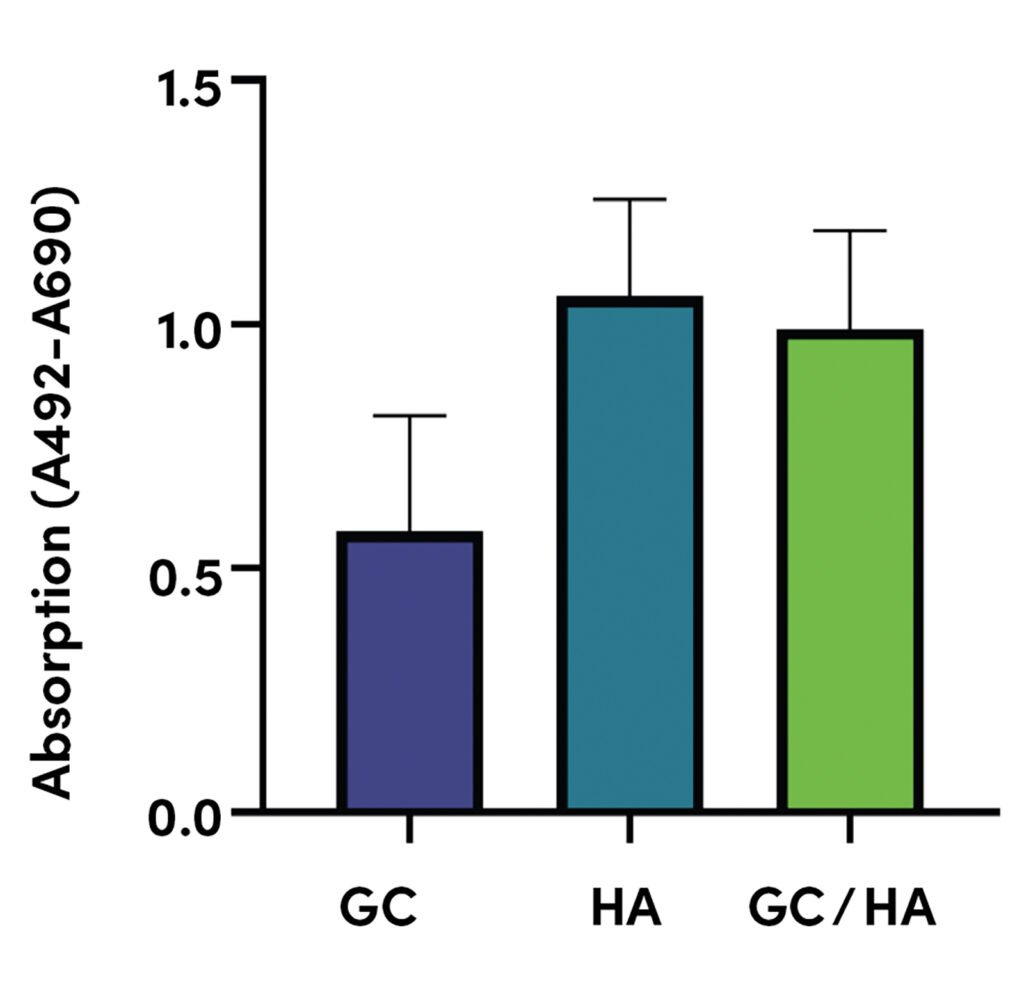
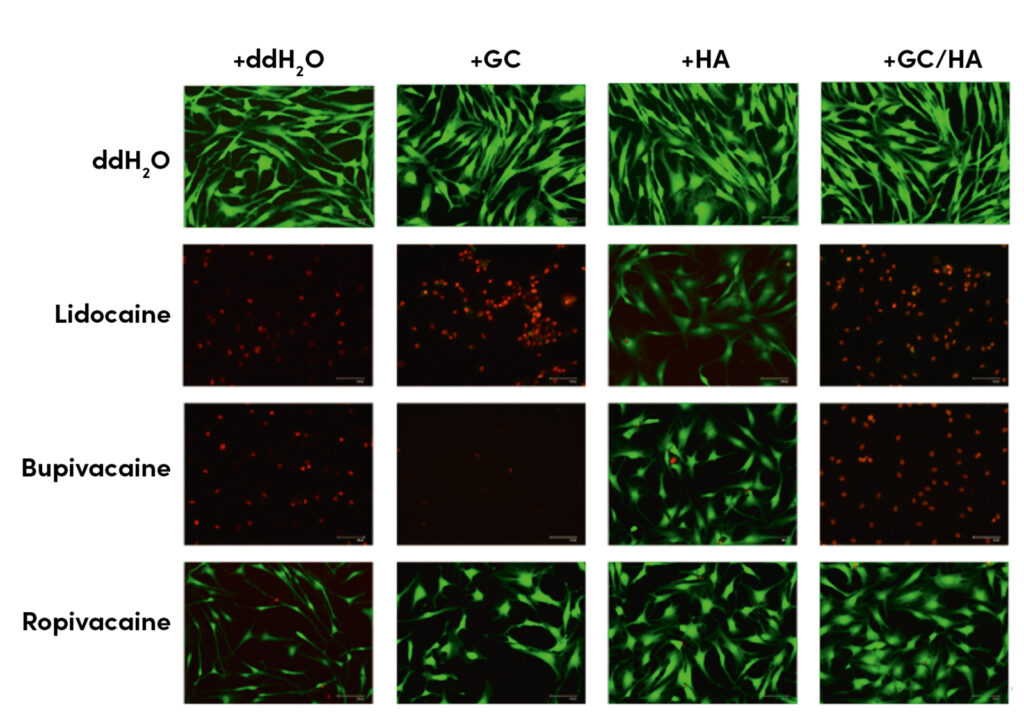
A similar study investigated the effects of combination therapy on arthritic human cartilage cells in a 2D cell culture [5]. Here, too, a significantly stronger chondroprotective effect was demonstrated, including reduced expression of cartilage-degrading genes and preservation of collagen type II synthesis and cell vitality. Another study also examined the effects of co-administration of hyaluronic acid with steroids and various local anesthetics in a human cell culture [6]. As can be seen in Figure 2, hyaluronic acid enhanced the positive effects of glucocorticoids while significantly reducing their cell-damaging effects, especially in combination with individual local anesthetics.
Conclusion
In summary, both clinical and preclinical studies suggest that the combination of hyaluronic acid with glucocorticoids represents a promising addition to conservative osteoarthritis therapy due to synergistic effects. The simultaneous use of both substances not only enables effective short-term symptom control, but also offers longer-term benefits by protecting the cartilage structure and cushioning the potentially adverse effects of steroids. For daily practice, this means that combined administration is a worthwhile, potentially safer, and more effective alternative to cortisone injections alone.
Literature
- Nakazawa F, Matsuno H, Yudoh K, Watanabe Y, Katayama R, Kimura T. Corticosteroid treatment induces chondrocyte apoptosis in an experimental arthritis model and in chondrocyte cultures. Clin Exp Rheumatol. 2002;20:773–81.
- McAlindon TE, LaValley MP, Harvey WF, Price LL, Driban JB, Zhang M, et al. Effect of intra-articular triamcinolone vs saline on knee cartilage volume and pain in patients with knee osteoarthritis a randomized clinical trial. JAMA – J Am Med Assoc. 2017;
- Hangody L, Szody R, Lukasik P, Zgadzaj W, Lénárt E, Dokoupilova E, et al. Intraarticular Injection of a Cross-Linked Sodium Hyaluronate Combined with Triamcinolone Hexacetonide (Cingal) to Provide Symptomatic Relief of Osteoarthritis of the Knee: A Randomized, Double-Blind, Placebo-Controlled Multicenter Clinical Trial. Cartilage. 2018;9:276–83.
- Bauer C, Moser LB, Kern D, Jeyakumar V, Nehrer S. The Combination of Glucocorticoids and Hyaluronic Acid Enhances Efficacy in IL-1β/IL-17-Treated Bovine Osteochondral Grafts Compared with Individual Application. Int J Mol Sci. 2023;24.
- Bauer C, Moser LB, Jeyakumar V, Niculescu-Morzsa E, Kern D, Nehrer S. Increased Chondroprotective Effect of Combining Hyaluronic Acid with a Glucocorticoid Compared to Separate Administration on Cytokine-Treated Osteoarthritic Chondrocytes in a 2D Culture. Biomedicines [Internet]. 2022;10. Available from: https://www.mdpi.com/2227-9059/10/7/1733
- Moser LB, Bauer C, Jeyakumar V, Niculescu‐morzsa EP, Nehrer S. Hyaluronic acid as a carrier supports the effects of glucocorticoids and diminishes the cytotoxic effects of local anesthetics in human articular chondrocytes in vitro. Int J Mol Sci. 2021;22.
Autoren
ist Assistenzarzt Orthopädie und Traumatologie an der Klinischen Abteilung für Orthopädie und Traumatologie, Universitätsklinikum Krems
(Dipl.-Ing. / PhD BSC BA), Senior Post-Doc - Masterstudium Biotechnologie & Bioanalytik und PhD in Regenerativer Medizin. Post-Doc - Zentrum für Regenerative Medizin, Universität für Weiterbildung Krems.
ist Facharzt für Orthopädie und orthopädische Chirurgie. Er leitet das Zentrum für Regenerative Medizin und das Department für Gesundheitswissenschaften, Medizin, Forschung an der Donau Universität Krems, samt Professur für Tissue Engineering. Daneben ist er am Uni-Klinikum Krems an der orthopädischen Abteilung, mit Schwerpunkt Sportorthopädie und Knorpelchirurgie tätig. Seit 1992 in der GOTS, war er u.a. bereits deren Präsident und Vizepräsident Österreichs und war 2025 Kongresspräsident des GOTS-Kongresses in Krems sowie Präsident der ÖGSMP (2022). Außerdem ist er wiss. Beirat der sportärztezeitung.
© UWK/Daniel Novotny